Morgan Mae’s NICU Miracle: From 66% Blood Loss at Birth to a Thriving One-Year-Old
- KimAnh
- April 21, 2026

A birth that became a fight for survival within seconds
Morgan Mae’s life did not begin with quiet celebration—it began with urgency.
Born prematurely at 33 weeks, Morgan entered the world under life-threatening circumstances. A rare and severe condition known as fetomaternal hemorrhage had caused her to lose an estimated 66% of her blood volume before birth. In simple terms, she arrived already fighting for survival.
As her tiny body struggled to compensate, she developed hydrops fetalis, a dangerous condition marked by abnormal fluid buildup around vital organs, including the lungs and heart. The combination of massive blood loss and fluid overload created a critical situation—one that left doctors uncertain whether she could survive.
There was no time to wait.
Emergency delivery and immediate intervention
An emergency cesarean section was performed to save Morgan’s life.
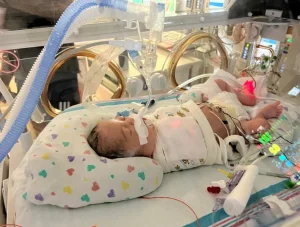
The moment she was delivered, a team of specialists began aggressive treatment. She required multiple blood transfusions to replace what she had lost, along with intubation to support her breathing.
To address the fluid surrounding her lungs and heart, doctors administered Lasix, a medication used to remove excess fluid from the body. Every intervention was carefully calculated, every decision urgent.
Morgan’s first hours were not about recovery—they were about stabilization.
A devastating setback: pulmonary hemorrhage
Just as her condition began to show signs of improvement, another crisis emerged.
When doctors attempted to remove her breathing tube—a step known as extubation—Morgan suffered a pulmonary hemorrhage, a severe and life-threatening bleed in her lungs.
In an instant, her fragile progress was undone.
She was reintubated and placed on a high-frequency oscillator, a specialized ventilator used in the most critical neonatal cases. This machine delivered rapid, precise breaths to protect her lungs while maintaining oxygen levels.
At that point, survival was uncertain.
Her parents were forced to confront a reality no family should face: that despite every effort, there were no guarantees.

“Slow and steady”: a fragile path to recovery
What followed was not a sudden turnaround—but a gradual, hard-fought recovery.
Morgan’s progress was described by her doctor in simple but powerful terms:
“Slow and steady.”
Those words became a mantra for her family.
Day by day, she began to stabilize. Her body responded to treatment. Her lungs slowly improved. Her vital signs became less volatile.
There were no dramatic breakthroughs—only incremental victories:
- a stable oxygen reading
- a successful feeding
- a quiet night without complications
Each small step forward carried enormous meaning.
63 days in the NICU—and a long-awaited homecoming
After 63 days in the Neonatal Intensive Care Unit (NICU), Morgan reached a milestone that once felt impossible:
She was strong enough to go home.
For her parents, the moment was overwhelming. What began as a life-threatening emergency had evolved into a journey of survival, endurance, and cautious hope.
They gave her a nickname that perfectly captured her path:
“Turtle.”
Not because she was slow—but because she never stopped moving forward.
Life after the NICU: challenges and progress
Morgan’s journey did not end when she left the hospital.
Like many premature infants who experience severe complications, she continues to face ongoing health challenges, including:
- sleep apnea
- hearing impairment
- motor development delays
Yet, these challenges exist alongside something far more powerful: her ability to thrive.
Her parents describe her as joyful, energetic, and full of life—a child whose personality shines far brighter than the medical history behind it.

The strength behind every milestone
For Morgan, progress is measured differently.
Each achievement—no matter how small—represents something extraordinary:
- learning to control her breathing
- gaining strength in her movements
- responding to sound and interaction
- engaging with the world around her
These are not ordinary milestones. They are victories earned through resilience, medical care, and unwavering support.
Her nickname, “Turtle,” has become more than a reflection of her pace—it is a symbol of her perseverance.
The emotional reality of NICU parenting
Behind Morgan’s medical journey is another story: her parents’ experience.
Her mother, Danielle, describes the NICU as a place of constant vigilance, emotional strain, and difficult decisions. Every day required balancing hope with uncertainty, strength with fear.
Parents in these situations become more than caregivers—they become advocates.
They learn medical language, monitor changes, ask questions, and make decisions under pressure. They celebrate progress that others might overlook, because they understand how fragile each step truly is.
Danielle’s reflection is clear:
advocacy, patience, and trust in both instinct and medical expertise were essential to Morgan’s survival.
A thriving one-year-old—and a story of hope
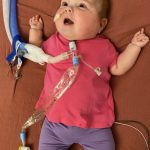
Now approaching her first birthday, Morgan Mae is thriving.
She laughs, plays, explores, and connects with the world in ways that once seemed uncertain. Her presence is filled with energy and joy—an embodiment of how far she has come.
For her family, every smile carries meaning.
Every giggle is a reminder of the days when even breathing was not guaranteed.
The role of medicine, family, and hope
Morgan’s story highlights the intersection of several critical forces:
- advanced neonatal medicine, capable of managing extreme cases
- dedicated NICU teams, providing round-the-clock care
- parental advocacy, ensuring every concern is heard
- emotional resilience, sustaining families through uncertainty
Together, these elements create the possibility of survival—and, in cases like Morgan’s, the chance to truly thrive.
Final reflection
Morgan Mae’s life began under the most fragile conditions imaginable.
She faced massive blood loss, organ stress, respiratory failure, and life-threatening complications within her first days. Yet through it all, she endured—step by step, breath by breath.
Her story is not defined by how fast she recovered.
It is defined by the fact that she never stopped moving forward.
Today, “Turtle” is no longer just a nickname.
It is a reminder that even the slowest progress can lead to extraordinary outcomes—and that resilience, when supported by love and care, can transform even the most uncertain beginnings into a life filled with joy.