Breaking: How a Multidisciplinary Pediatric Cardiac Team Saved Baby Joshua Castro’s Life Through Expertise, Precision, and Unwavering Family Devotion
There are moments in medicine when timing, teamwork, and trust align so precisely that they change the course of a life forever.
For baby Joshua Castro, that moment began long before he was born.
A Diagnosis That Changed Everything
When Jackie and Jason Castro discovered they were expecting their second child, their home was already filled with the laughter of their four-year-old daughter, Ellie. The pregnancy was meant to be a joyful continuation of their growing family.
But early bloodwork introduced an unexpected reality.
Doctors identified a high probability that their unborn son would have Down syndrome—a diagnosis confirmed on November 1, 2023. What followed was not panic, but preparation.
Rather than retreating into fear, the Castro family leaned forward. They sought out other families, built a support network, and began educating themselves on what lay ahead. It was a deliberate decision—to meet uncertainty with knowledge and community.
Still, more challenges were coming.
At 20 weeks, during a detailed anatomy scan, specialists identified a serious congenital heart defect: an atrioventricular septal defect (AVSD), a condition involving holes between the heart’s chambers that disrupt normal blood flow.
In that moment, the family’s journey shifted again—from preparation to urgency.
The Power of Early Intervention
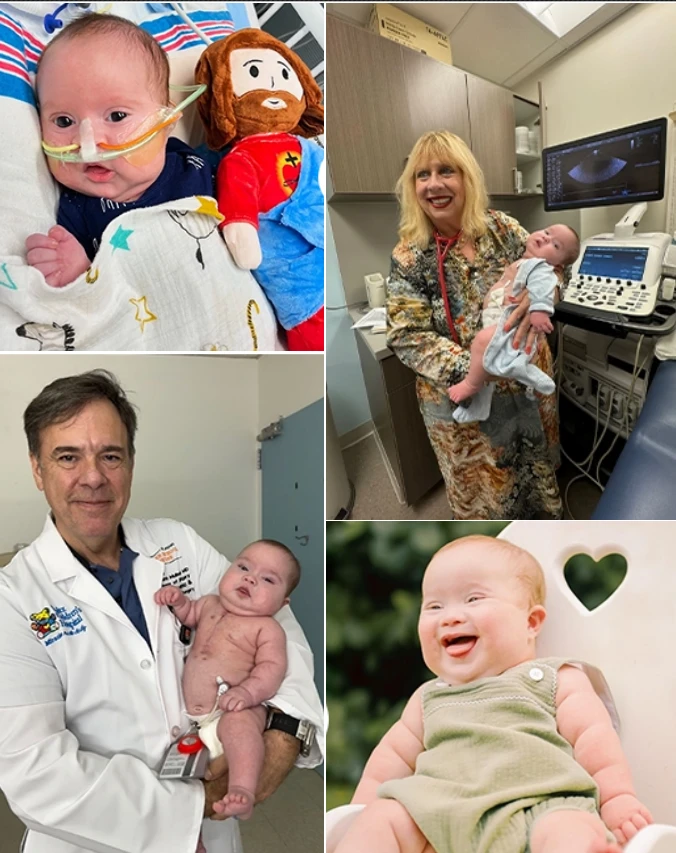
Under the care of Dr. Madeleen Mas, medical director of pediatric cardiology at UHealth Jackson Children’s Care, Joshua’s condition was closely monitored.
The value of early diagnosis quickly became clear.
“Prenatal detection allows families to prepare for major complications and can directly impact surgical outcomes,” Dr. Mas explained.
That preparation proved critical.
Throughout the pregnancy, Jackie underwent regular monitoring while the medical team mapped out a detailed plan for Joshua’s birth and immediate care. By the third trimester, the family had toured the hospital, met surgical specialists, and developed a level of trust that would soon become essential.
Among those specialists was Dr. Leonardo Mulinari, chief of pediatric and congenital heart surgery—a key figure in what would become a life-saving collaboration.
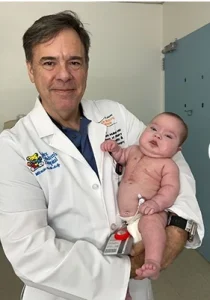
A Fragile Beginning
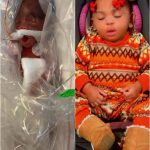
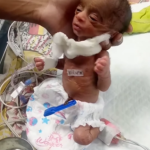
Joshua was born on April 10, welcomed into the world with cautious optimism.
He spent his first 23 days in the Neonatal Intensive Care Unit (NICU), where doctors monitored his condition closely. When he was finally discharged, the moment felt like a victory.
But it didn’t last.
Just three days later, Joshua began struggling to breathe.
He was rushed back—this time to the Pediatric Intensive Care Unit (PICU) at Holtz Children’s Hospital—where the reality of his condition fully emerged. He was placed on oxygen, connected to monitoring systems, and fitted with a PICC line for critical care.
This was no longer a waiting game.
It was a race against time.
A Series of Critical Interventions
On May 22, Joshua underwent his first major procedure to close a patent ductus arteriosus (PDA), a condition that was placing additional strain on his already compromised heart.
But even that was only part of the solution.
By early June, doctors identified excessive blood flow to his lungs, making breathing increasingly difficult. To stabilize him, Dr. Mulinari performed a pulmonary artery banding procedure—essentially buying Joshua time.
Time to grow.
Time to gain strength.
Time to survive long enough for the surgery that would ultimately save his life.

Setbacks That Tested Every Limit
The months that followed were some of the most difficult.
Joshua faced repeated hospitalizations, battling COVID-19, viral infections, fevers, and even a blood infection. Each complication threatened to undo the fragile progress he had made.
He required antibiotics, blood transfusions, and eventually a gastric feeding tube to support his nutrition and growth.
For the Castro family, these were not isolated incidents.
They were part of a relentless cycle—hope followed by setback, progress followed by uncertainty.
Yet through it all, Joshua endured.
Healing Beyond Medicine
While the medical team worked to stabilize Joshua physically, another group stepped in to support the family emotionally.
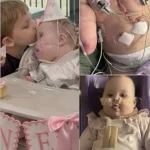
The child life team at Holtz Children’s played a critical role—especially for Ellie.
Through educational tools and even a stuffed animal designed to replicate Joshua’s heartbeat, they helped her understand her brother’s condition and stay connected during long hospital stays.
It was a reminder that healing is not only clinical.
It is emotional.
It is human.

The Surgery That Changed Everything
By September, Joshua had reached a critical milestone—he weighed just over 5 kilograms, enough to proceed with open-heart surgery.
On September 17, the operation began.
Using cardiopulmonary bypass, surgeons temporarily took over the function of Joshua’s heart and lungs, allowing them to repair the defects. The pulmonary artery band was removed, and a patch was placed to close the holes in his heart.
The procedure was complex.
The risks were high.
But the outcome was extraordinary.
Joshua was extubated the very same day—a sign of remarkable stability.
A Recovery That Defied Expectations
Just five days after surgery, Joshua went home.
For a child who had spent months in and out of intensive care, the speed and success of his recovery were nothing short of remarkable.
Dr. Mas later described the case as one of the best outcomes she had seen in her 34-year career—crediting not just the surgical success, but the seamless coordination between specialists, nurses, therapists, and support staff.
This was the power of a multidisciplinary team in action.
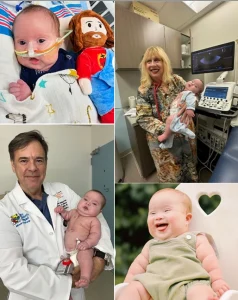
A Journey That Continues
Joshua’s story does not end with surgery.
He will continue to receive care from a wide network of specialists, including cardiology, neurology, genetics, and gastroenterology. He will also participate in therapies designed to support his speech, movement, and overall development.
The road ahead remains complex.
But it is no longer uncertain in the same way.
There is a plan.
There is progress.
There is hope.
A Testament to Collaboration and Love
For Jackie, the experience has been transformative.
“They didn’t just care for Joshua,” she said. “They cared for our entire family.”
That distinction matters.
Because Joshua’s survival was not the result of a single moment or a single decision. It was the result of preparation, expertise, and a network of people working together toward one goal.
To give a child a chance.
A Story That Inspires Beyond the Hospital Walls
Joshua Castro’s journey stands as a powerful reminder of what modern medicine—and human compassion—can achieve together.
It highlights the importance of early diagnosis.
The life-saving impact of coordinated care.
And the unshakable strength of families who refuse to give up.
Because in the end, this is not just a story about a heart defect.
It is a story about what happens when science, dedication, and love come together at exactly the right moment.
And for Joshua, that moment made all the difference.